IVF - In Vitro Fertilization (Test Tube Baby)
IVF - Test Tube Baby
Anything which occurs outside the body is called in vitro and when fertilization of egg with sperm occurs outside the body it is called "IN VITRO FERTILIZATION". The first In Vitro fertilization was done in the test tube and that is why it is popularly known as Test tube Baby.
The process of fertilization which normally in fallopian tube of the woman and the fertilized egg than moves into the uterus of the woman.
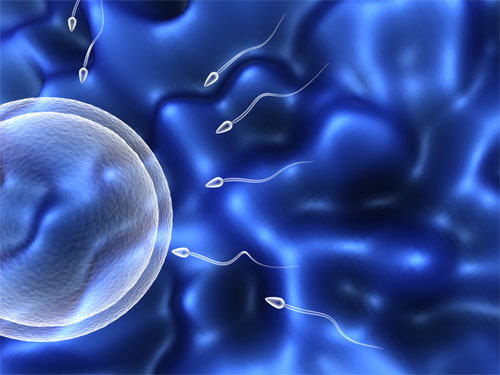
It an implants there in to the uterus and developed into the baby. When for some reason this process of fertilization cannot take place naturally or sperm and egg cannot be transported naturally to the tube or from the tube to the uterus or either is egg having some problem or the sperm.
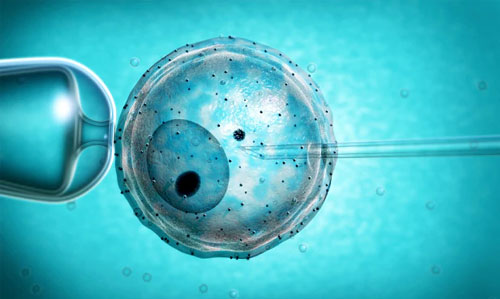
Some problem in fertilization during test tube baby process we need to asses the fertilization to help fertilization we take out of the egg from the wife of egg from the woman's ovary and in control lab and environment we fertilized egg with the help of sperm of her male partner. After fertilization the fertilized egg are cultured into the control laboratory environment to form pre-embryos and this pre-embryos are then transferred back into the uterus of the woman. If they implant and grow become the pregnancy, and hence test tube baby is most convenient process.
IVF - Step by Step
Preliminary Testing: This includes first consultation, blood tests culture if necessary, hysteroscopy, D21 visit i.e. mock transfer trial, semen freezing and serum progesterone.
First Consultation: We will complete a history and physical examination of both partners. Transvaginal sonography of female partner and semen examination of male partner and culture of it, if necessary. It is helpful to bring of your old medical reports, if available.
Base Line Blood Investigation: This includes D3 FSH, LH, PRL, TSH, Major pre operative profile and other special blood investigations if necessary. This will help us to choose best stimulation (Medication) protocol to complete your IVF cycles.
Hysteroscopy: If you have previously had a hysteroscopy please bring their reports. This test must be scheduled to be completed on days 5-11 of the menstrual cycle. Menstruation must be absent for this test to be done.
D21 visit:
Semen freezing
Mock transfer trial
Serum progesterone
TVS
Semen Freezing: It is necessary to freeze a semen specimen before your IVF cycle starts. This sample is used only as an emergency back up for the day of retrieval. We prefer to inseminate the eggs with fresh semen if possible. We will discard the sample after completion of cycle except if you choose to have another IVF cycle.
Transvaginal sonography will tell us thickness of endometrium on D21.
Serum progesterone level estimation.
Mock transfer trial: Embryo transfer is very important procedure and it is usually done without anesthesia so, on day 21 we will do mock embryo transfer to anticipate any difficulty and solution far it before actual transfer. It is painless procedure.
Development of Oocytes (Eggs)
It is necessary to stimulate the ovary to produce multiple follicle (the sac that contains the egg), in order to improve your chances of a successful outcome from an IVF cycle. After the consult with the doctor, you will receive prescription for a specific type of medication stimulation protocol. There are many different medication protocols that the doctor may prescribe for you. This decision is based on factors such as your age, infertility history, a past response to these medications, and a base line FSH level. The fertility medications that are necessary to stimulate the ovary are unfortunately all inject able medications. Doctor and nurse will explain you the dosage and method of administration.

Fertility Medication: If we have more than one egg we have better chance of pregnancy of in IVF cycle. To get more eggs we stimulate the ovaries with stimulation drugs called gonadotrophins. Gonadotrophins can be manufactured from urine or by recombinant DNA technology. Appropriate type of gonadotrophins and dose of administration are selected for individual patients. Available gonadotrophins include HMG, FSH and recombinant FSH manufactured by different pharmaceuticals.
Side Effect of Fertility Medication:
Over stimulation of the ovary, It can occur to varying degrees: mild, moderate or severe.
Multiple Births: The risk of conceiving a multiple pregnancy during and IVF cycle is dependent upon your age, response to the medications, the quality of the embryos, the number of embryos replaced into the uterus and other unforeseen factors are considered when judging your specific risk of multiple births.
Common Complaints: Pain at the injection site, headaches and fatigue.
Special Note: You may have read reports that fertility drugs increase the risk of ovarian cancer. To date there are no conclusive studies that identify an association between taking fertility drugs and ovarian cancer.
GnRH analog (Lupride): This medication is administered by subcutaneous injection. It is given to prevent premature release of the oocytes (eggs). Side effects may include: localized skin reaction, allergic reaction, headaches, hot flashes and mood swings. If your scheduled menstruation is late while on Lupron, you should have a pregnancy test.
HCG (Human Chorionic Gonadotropin): You will be given instruction for the exact time of this injection. It is generally taken 34-36 hours prior to the egg retrieval. This medication should be injected into the muscle. This medication completes the maturation of the egg.
Progesterone: You will begin talking this naturally occurring hormone on the next to egg retrieval. This medication, assist the embryo to attach to the uterus. The side effects that have been reported include: breast tenderness, headache, nausea, fluid retention, fatigue, mood swings, depression, pain at the site of injection (in the case of inject able progesterone). Vaginal itching and irritation (in the case of vaginal form). If you have a history of blood clots or thrombophlebitis you should alert the medical staff.
Oocyte (Egg) Retrieval: The egg collection process (retrieval) is usually accomplished using the Ultrasound-guided trans vaginal method. Other methods of retrieving oocyte that are rarely utilized in our practice but are sometimes necessary, include Laparoscopy or a Trans-Abdominal approach.
This ultrasound-guided trans vaginal method of egg retrieval allows this procedure to be done in an out patient setting. A vaginal ultrasound allows for visualization of both ovaries. A needle is inserted through the vaginal wall in the ovary. Each follicle is punctured individually and the fluid containing the egg is examined by the embryologist under the microscope until the egg is found. The duration of this procedure is usually less than 45 minutes.
This procedure is done under general anesthesia.
Sperm Collection and Insemination: While the egg retrieval is underway, you will be notified by the andrology/embryology staff that a sperm sample is needed. The specimen will be processed in our laboratory and prepared for egg insemination. Please discuss with the embryology staff if any question or concern you may have prior to the day of egg retrieval. Frozen specimen collected will be used only in case of emergency (illness, inability to procedure a specimen etc.)
Incubation and Fertilization of Oocytes (Eggs): The eggs and sperm will be placed together in a special culture fluid and kept in incubators in our laboratory. This procedure is called insemination.

Formation and Cleavage of Embryos: The eggs will be examined 16-20 hours after insemination for signs of fertilization. If fertilization occurs, the fertilized eggs are now described as pre-embryos or zygotes. When they divide to at least 2 cells they are called embryos. The laboratory environment is conducive for fertilization to occur, however, it cannot be guaranteed that fertilization will occur. Typically, 60% of the eggs retrieved will be fertilized. This percentage may be higher or lower depending on each couple.
Embryo Transfer: Embry transfer (ET) usually occurs forty eight to seventy two hours post retrieval. The time of transfer will be designated by the IVF staff. The embryo(s) that is (are) assessed to be developing normally will be considered for transfer. Although a recommendation (3-5 embryos) will be made regarding the number to transfer, the final decision resides with the couple and the doctor. Transferring multiple embryos may result in the growth of more than one foetus. If you have extra embryos after the transfer, they will be cryopreserved if they have demonstrated appropriate development.
The method used for transferring embryos is similar to that of the mock transfer. ET is performed by inserting a small catheter through the cervical opening into the uterine cavity. The embryo transfer is usually a painless procedure. There is a recommended rest period after the transfer. You will be given specific instruction prior to the transfer regarding your medications, future testing dates and activity restrictions.
Within 13 days post-transfer, hormonal levels and a pregnancy test will be done. If a pregnancy has occurred, further blood testing blood work and ultrasound will be required to assess normal progression.
Cropreservation (Freezing) Programme: The purpose of embryo freezing programme is to give a couple participating in the IVF programme the best chance to achieve a pregnancy with a maximum of safety. At the end of an IVF cycle there are often multiple embryos available for transfer. It has been found that transferring more than four embryos caries a significant risk of multiple pregnancies, while it does not increase the singleton pregnancy rate proportionately. The advantage of cryopreservation is that there may be an increased chance of pregnancy without the necessity of multiple stimulation cycles and oocyte retrievals.
The frozen embryo transfer takes place in an identical manner to a fresh embryo transfer.
Embryo selected for cryopreservation will be frozen up to three days after the egg retrieval. The embryos will be placed in a cryopreserved media and frozen in a step-wise manner. At the end of the cryopreservation procedure the embryos will be stored frozen in tanks filled with liquid nitrogen. Brought back to normal life. There is no guarantee of the survival of human cryopreserved thawed embryos. If they have not survived (as seen at the time of thawing), they will not be transferred. We consider couples whose eggs and sperm become an embryo to be the owners and persons who control their embryos in the test tube baby process. However, there is a time limit on this ownership and control.
For more details on our IVF Treatment, please visit our Hospital for proper Diagnosis & Treatment options.
Subsequently, you can Email your Queries at kanjeets@yahoo.com
